CLINUVEL’s expanded pharmaceutical research and development program is aimed at the translation of its technology and know-how developed and gained over the last decades, to serve wider populations. The medical needs of these patient populations have remained unmet, implying that no current therapy exists for these patients and no products have been developed for broader target populations. CLINUVEL frequently reports on the direction and clinical opportunities in which it seeks to test its drug candidates. In brief, a number of indications are reviewed below.
Erythropoietic Protoporphyria and SCENESSE® Enfance
We continue to develop the application of an afamelanotide formulation for paediatric patients diagnosed with the rare metabolic disorder, erythropoietic protoporphyria (EPP). A focus of the research is the assessment of different formulations of SCENESSE® based on four age groups. The research in the Singapore based Research, Development & Innovation Centre (RDI) is being conducted by senior managers under the direction of the Chief Scientific Officer.
Vitiligo
Vitiligo is a common skin depigmentation disorder which affects between 0.1-2% of the world’s population. The pigment producing cells of the skin (melanocytes) are either no longer functional or in some cases absent as a result of a variety of factors. As a result, the human skin – over time – starts to develop lighter depigmented patches of skin (vitiligous lesions) which appear across the surface of the body. The disease is resistant to treatment and has an intense psychological and social impact on these patients. Its devastating effect is most pronounced for patients of darker skin complexion.
CLINUVEL has successfully evaluated the efficacy of SCENESSE® in conjunction with narrowband ultraviolet B (NB-UVB) phototherapy as a systemic treatment for the repigmentation of darker skin types. Also being developed through the Singapore RDI are topical pharmaceutical formulations of melanocortin analogues (such as CUV9900) for the treatment of vitiligo and various other conditions.
CLINUVEL has undertaken studies in the past (Phase II CUV102 in 2011 and Phase IIb CUV103 in 2014) which produced encouraging results on repigmentation with SCENESSE® in conjunction with NB-UVB phototherapy. These results are accessible through the CLINUVEL website. As a next step in the drug development path, CLINUVEL plans to commence a Phase II study in North America with a focus on people with Fitzpatrick skin types IV-VI whose need for repigmentation is greatest. Their darker skin pigmentation shows the most distinct improvement, and therefore benefit, from treatment.
We have continued to liaise with the US Food and Drug Administration (FDA) on an agreed design of the study.
Of importance was that in March 2021, for the first time in its history, the FDA held a public meeting on patient-focused drug development for vitiligo with 1,155 participants. The focus on the disorder is welcomed and indicated the demand for novel treatments, only 24% of the participants stated that they would not use a daily topical treatment that provided only up to 50% repigmentation.
A global update on the stages of the development progress to take SCENESSE® to a prospective vitiligo market is provided below:
- Agreement on design;
- Recruitment of centers and participants;
- Undertake and complete the study ;
- Post study analysis and sharing of results with the FDA;
- Completion of additional research considered necessary;
- Submission and assessment of a Supplementary New Drug Application;
- Regulatory decision;
- Establishment of distribution and reimbursement arrangements; and then,
- First treatment.
A minimum time frame of three years is a realistic expectation to travel this path to first treatment but depends on the clinical results and regulatory authorities; the Company will provide periodic updates on its progress for the information of stakeholders.
DNA Repair and XP
Due to the frequency and length of UV exposure, large groups of the global population are at risk of permanent skin damage, called photodamage, and high percentages progress to solar skin damage and first stages of skin cancers. The risk of skin cancers following UV exposure is the highest in those who are deficient in their natural DNA repair processes, specifically base-excision repair (BER), and nucleotide-excision repair (NER).
Going deeper in the subject, UV and HEV light impacts cellular DNA, causing chemical alterations to DNA – the preliminary step in cancer formation.
In clinical testing, afamelanotide has been shown to reduce DNA damage caused by UV radiation and visible light (oxidative damage and pyrimidine dimers). Further research has shown the ability of afamelanotide and other melanocortin molecules to assist skin cells in DNA repair mechanisms (such as NER).
The Company announced the DNA Repair Program in September 2020 with an initial focus on xeroderma pigmentosum (XP) patients who are >1,000 times more susceptible to skin cancers than the general population.
The prevalence of XP ranges from 1:250,000 to 1,100,000 in western populations.
The fist XP-C variant patient in the world was treated in September 2020 and tolerated the drug well during a 42 day observation period, thus providing the basis to progress to the planned study. This study is the first-ever to have been approved by Ethics Committee(s) in western countries, as – due to the fatal course of the disease – the concern has been to protect XP patients from human medicinal trials and experiments.
The scope of the XP study was subsequently extended in 2021 to XP-V variant patients.
A number of studies have been designed in collaboration with expert physicians. We share three of these at this stage – CUV150, 151 and 152 – while reviews are performed by regulatory authorities and Ethics Committees. Individual patients have provided consent for the studies to commence.
The global objectives are to evaluate afamelanotide, a first-in-class melanocortin – in XP-C and XP-V patients in relation to safety, the effect on the integrity of the skin, photoproducts, NER and overall, as a systemic photoprotective drug.
| Clinical trial | Phase | Target population | Participants |
|---|---|---|---|
| CUV150 | Phase IIb | XP-C | n=6 |
| CUV151 | Phase II | Healthy volunteers | n=10 |
| CUV152 | Phase IIb | XP-C and XP-V | n=6 |
These involve the administration of the drug over four months, skin biopsies to assess UV damage, and the administration of ultraviolent radiation to assess the effect of erythemal exposure.
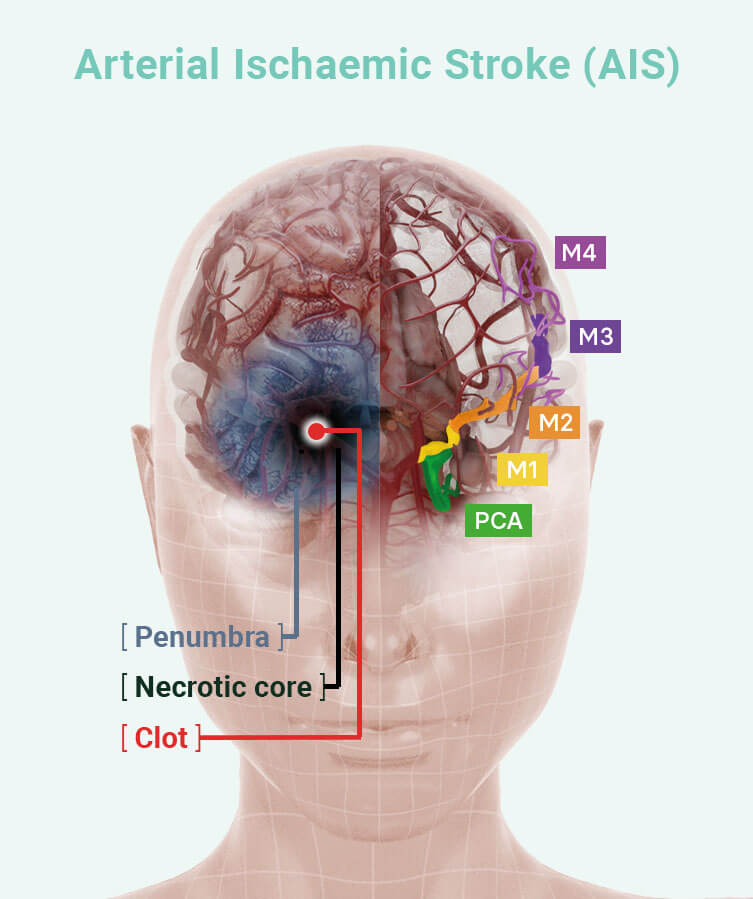
Stroke – AIS
Stroke impacts 15 million people worldwide each year. Of these, 85% (12.75 million) are arterial ischemic stroke (AIS), around 85% (10.84 million) of which are untreatable due to the blood clot prevailing in narrow and inoperable blood vessels of the brain.
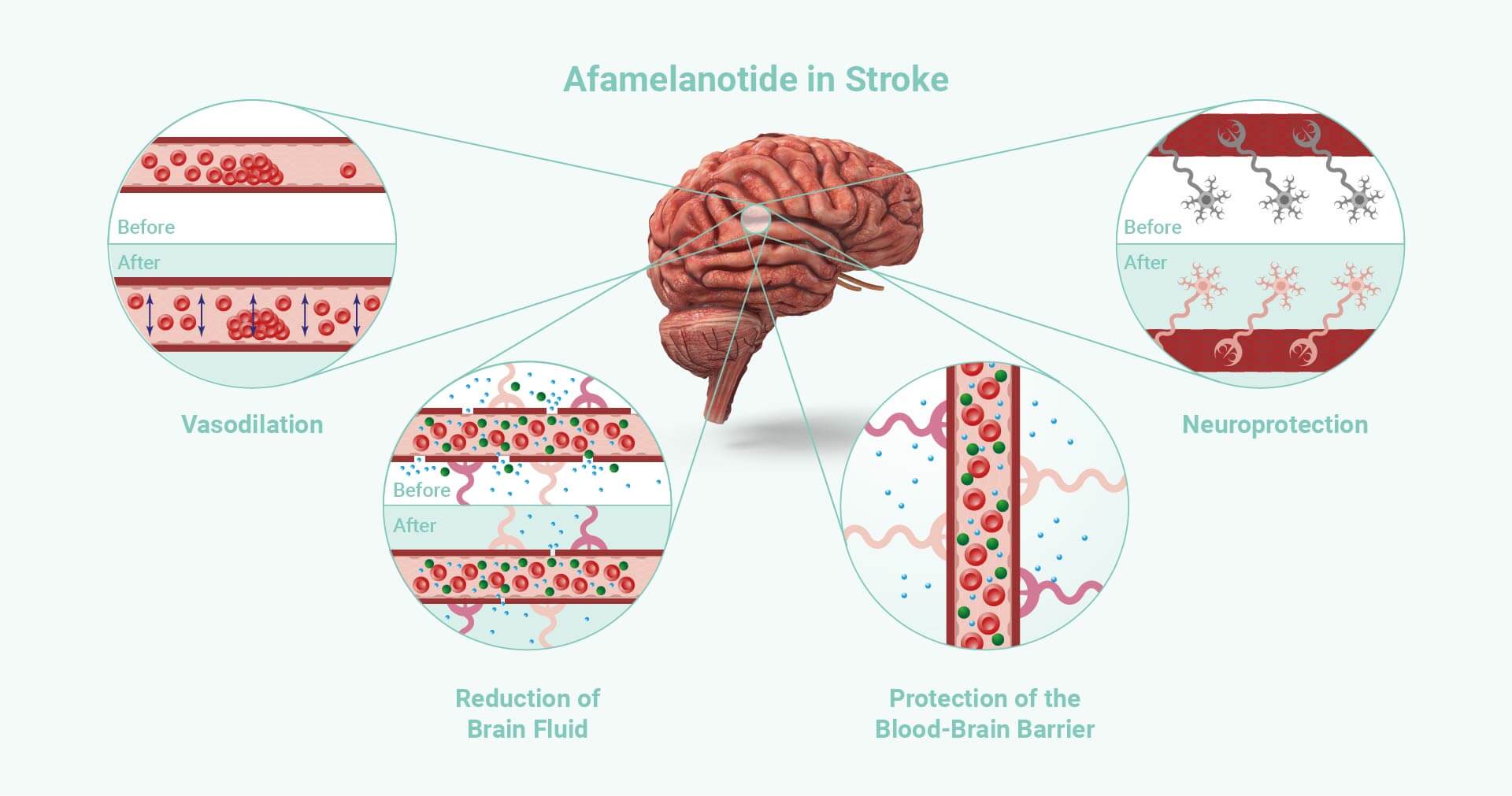
Afamelanotide assists blood vessels to stimulate blood flow and oxygen to the penumbra, the brain tissue at risk; it also provides protection of the brain cells.
A Phase II study – CUV801 has been designed and approved by clinical decision makers and ethical committees and commenced.
The first of six AIS patients was treated in June 2021, conducting the world’s first human study of a systemic melanocortin in the treatment of a life-threatening condition.
The objective is to assess whether afamelanotide’s intervention provides a benefit to the arterial supply of the brain as measured by Computed Tomography Perfusion and Magnetic Resonance Imaging of the brain.
Progress of the study will be advised.
Additional Indication
We are also working towards institutional agreements to start a first study in an additional indication.